Certification in Spinal
Manipulative Therapy
4 courses | 60 hours
FSBPT, ProCert, BOC & APTA approved
Diploma in
MSK Ultrasonography
4 courses | 60 hours
Includes RMSK Registry Exam Preparation & Review
Fellowship in
MSK Ultrasonography
6 courses | 114 hours
Spine, Extremities & Regenerative Medicine Applications

The Certification in Spinal Manipulative Therapy (Cert. SMT) credential consists of 60 hours of hands-on training in exclusively high-velocity low-amplitude thrust manipulation techniques of all spinal and pelvic articulations. Four courses comprise this certification: SMT-1, SMT-2, SMT-3 and SMT-4. All courses are approved by the Federation of State Boards of Physical Therapy (FSBPT), BOC and ProCert.

The Certification in Dry Needling (Cert. DN) credential consists of 54 hours of hands-on and didactic training in dry needling techniques, safety and evidence for craniofacial, cervicothoracic, upper extremity, lumbopelvic and lower extremity conditions. Two courses comprise this certification: DN-1 and DN-2. All courses are approved by the Federation of State Boards of Physical Therapy (FSBPT), BOC and ProCert.

The Diploma in Osteopractic consists of 178 hours of post-graduate training in spinal and extremity high-velocity low-amplitude thrust manipulation, dry needling, instrument-assisted manual therapies and differential diagnostics for the management of neuromusculoskeletal conditions. All courses are approved by FSBPT, BOC and ProCert. Successful completion permits use of the Osteopractor title.

The Vestibular Concussion Specialist Certification (Cert. VCS) consists of 30 hours of hands-on and didactic training in the differential diagnosis and management of sports-related concussions and high/low level patients with all types of dizziness disorders. All courses are approved by FSBPT, APTA, and BOC.

Certification in Blood Flow Restriction (Cert. BFR) will be awarded after successful completion of this two-day (15-hour) course in blood flow restriction (BFR) rehabilitation and performance training. Participants will learn to utilize a variety of BFR devices and techniques to maximally enhance patient recovery and client performance. All courses are approved by FSBPT, APTA, and BOC.
The AAMT Fellowship is accredited by the APTA as a post-professional fellowship program for physical therapists in orthopaedic manual physical therapy. Graduates of the 12-month distance-based AAMT Fellowship are awarded the FAAOMPT credential.
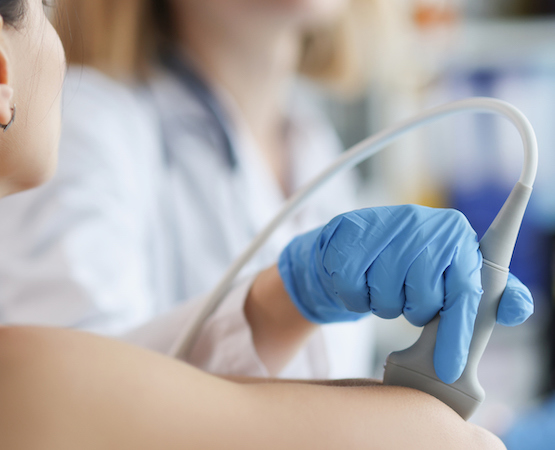
The Certified Musculoskeletal Ultrasonographer credential consists of 30 hours of didactic, technical and hands-on training in the essential components of diagnostic musculoskeletal ultrasound of the upper and lower extremities. Two courses comprise the Cert. MSK Sonographer credential: MSKU-1 (Diagnostic MSK Ultrasonography of the Upper Extremities) and MSKU-2 (Diagnostic MSK Ultrasonography of the Lower Extremities).
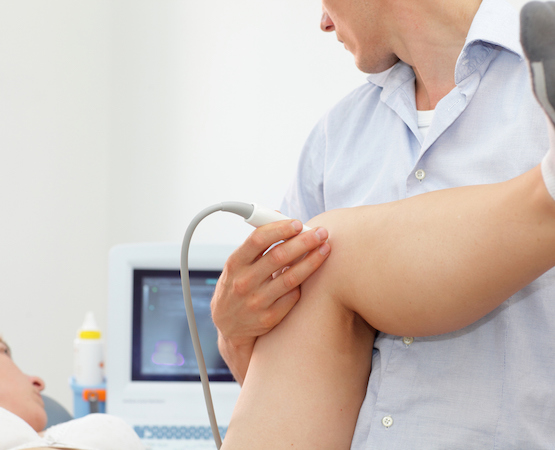
The Diploma in Musculoskeletal (MSK) Ultrasonography consists of 60 hours of didactic, technical & hands-on training. Four courses comprise the Diploma in MSK Ultrasonography: MSKU-1 (Diagnostic MSK Ultrasonography of the Upper Extremities), MSKU-2 (Diagnostic MSK Ultrasonography of the Lower Extremities), MSKU-3 (Rheumatology, Oncology, and Physics in Musculoskeletal Ultrasound), and MSKU-4 (Advanced Musculoskeletal Sonography & RMSK Registry Exam Review).
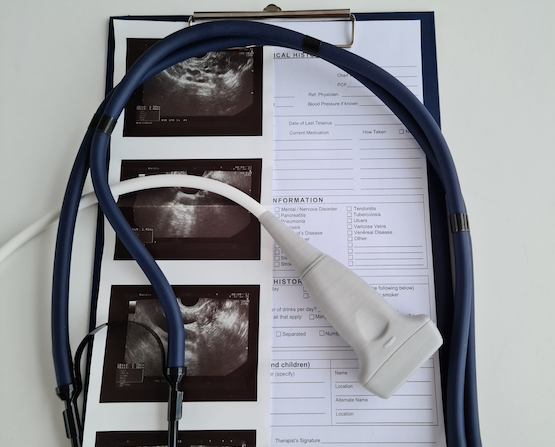
The Fellowship in MSK Ultrasonography consists of 114 hours of didactic, technical and hands-on training. Six courses comprise the Fellowship: MSKU-1 (Diagnostic MSK Ultrasonography of the Upper Extremities), MSKU-2 (Diagnostic MSK Ultrasonography of the Lower Extremities), MSKU-3 (Rheumatology, Oncology, and Physics in Musculoskeletal Ultrasound), MSKU-4 (Advanced Musculoskeletal Sonography & RMSK Registry Exam Review), MSKU-5 (Diagnostic MSK Ultrasonography of the Spine), and MSKU-6 (Regenerative Medicine Applications).

The Worldwide Leader in Spinal Manipulation & Dry Needling Education.
What is an Osteopractor?
An Osteopractor is a physical therapist, medical doctor, or doctor of osteopathic medicine that has completed an evidence-based post-graduate training program in the use of spinal and extremity thrust manipulation, ultrasound-guided dry needling, instrument-assisted manual therapies, and differential diagnostics for the diagnosis and treatment of neuromusculoskeletal conditions.
Osteopractic Physical Therapy is an approach to care, a sub-specialty within physical therapy, and more accurately describes the kind of physical therapy services offered (rather than simply “physical therapy”) so the public, potential patients, and colleagues alike, can identify the appropriate practitioner of choice for the condition in question. When you break a bone, you look for an orthopedist, not just a general medical doctor….
Become an Osteopractic Physical Therapist by learning spinal manipulation, extremity manipulation, dry needling, instrument-assisted soft-tissue mobilization, and differential diagnostics from the experts! The American Academy of Manipulative Therapy is dedicated to teaching physical therapists, osteopaths and medical doctors the science and art of thrust manipulation and dry needling.
What is an Osteopractor?
An Osteopractor is a physical therapist, medical doctor, or doctor of osteopathic medicine that has completed an evidence-based post-graduate training program in the use of spinal and extremity thrust manipulation, ultrasound-guided dry needling, instrument-assisted manual therapies, and differential diagnostics for the diagnosis and treatment of neuromusculoskeletal conditions.
Osteopractic Physical Therapy is an approach to care, a sub-specialty within physical therapy, and more accurately describes the kind of physical therapy services offered (rather than simply “physical therapy”) so the public, potential patients, and colleagues alike, can identify the appropriate practitioner of choice for the condition in question. When you break a bone, you look for an orthopedist, not just a general medical doctor….
Become an Osteopractic Physical Therapist by learning spinal manipulation, extremity manipulation, dry needling, instrument-assisted soft-tissue mobilization, and differential diagnostics from the experts! The American Academy of Manipulative Therapy is dedicated to teaching physical therapists, osteopaths and medical doctors the science and art of thrust manipulation and dry needling.
Get Certified in Spinal Manipulative Therapy & Dry Needling through the Worldwide Leaders
Get Certified in Spinal Manipulative Therapy & Dry Needling through the Worldwide Leaders
Osteopractic Physical Therapy

Osteopractic Physical Therapy
-
El Paso, TX
"Dr. Dunning is the real deal; he can manipulate extremely well. He knows the evidence and dispels many of the myths and misconceptions about traditional manual therapy approaches. I recommend these osteopractic manipulation courses to all physical therapists, especially Fellows who want to become experts in spinal manipulation technique."
-
Louisville, MS
"Dr. Dunning's dry needling course is far beyond just inserting needles into trigger points within muscles. Needling techniques are demonstrated for the direct treatment of tendons, ligaments, musculotendinous junctions, teno-osseus junctions and peri-neural stimulation. In addition, a comprehensive review of the literature underpinning the use of dry needling in musculoskeletal practice is given. I highly recommend this osteopractic dry needling course for all physical therapists interested in improving outcomes of patients with neuromusculoskeletal conditions."
-
Smithfield, NC
"Dr. James Dunning is an excellent lecturer, superb demonstrator and marvelous manipulator. His knowledge of the relevant spinal manipulation literature is extraordinary. I intend to does this course and the spinal manipulation techniques justice in my medical practice."
-
Dyess Air Force Base, Abilene, TX
"My patients need spinal manipulation in certain situations. As a medical physician, I need to have the humility to know when medication is making a difference and when it is not. On this course, I learned how to effectively treat a variety of musculoskeletal pain syndromes with specific spinal manipulation procedures."